Fascia and Interstitium: An Expert’s Perspective

We are proud to bring you this interview about the fascia with Scott Dolly MS, ATC, CSCS. Scott is the owner of Evolution Human Performance and Rehabilitation in Winchester, VA. He has a Masters Degree in Athletic Training and practices movement analysis, manual therapy and functional fitness training. The interview has been edited for clarity and brevity.
Dr. Larson: So we’ve known each other for a long time Scott. You actually did a rotation with me in my orthopedic clinic while you were working on your Master’s degree! Now you’ve been in the real world for years; you’ve taken your training and moved so far beyond the basics! You’ve really become an expert in the fields of functional fitness, manual therapy, and treatment of myofascial disorders. I know you’ve been an instructor for Hawkgrips IASTM for several years now. What else have you been working on lately?
Scott: Yeah, it’s really gotten crazy! Evo-HPR has grown into a 10,000 sqft space. We’ve had clients fly-in all the way from places like Los Angeles, Salt Lake City, and Alberta, Canada. And I’ve been lecturing and seeing clients internationally for 4-years now with RUNGA. People can check that out at www.rungalife.com. I’ve also worked with the Spartan Pro-Team for Spartan Race. And I’ve been featured on the Ben Greenfield Podcast and a couple others. Things have been great!
Awesome! But let’s get down to the business at hand and the reason I wanted to talk with you today. Now in the past couple months, fascia and interstitium have been making headlines. This all started with a report on a movement to classify the interstitium as an organ in its own right. But that would make it the single largest organ in the body! Obviously, something has changed in our understanding of the interstitium. And I want to talk about that, but first, let’s get some basics down.
What’s the difference between interstitium and fascia?
Fascia and the interstitium are alike in many ways and may not be that different at all. Being able to identify what makes them different is going to be key in truly defining the interstitium as a new organ. For now, the only difference that exists between them may just be semantics. Dr. Kumka and Dr. Bonar published one of the best articles on the topic It was published back in back in 2012 and titled “Fascia: a morphological description and classification system based on literature review.”
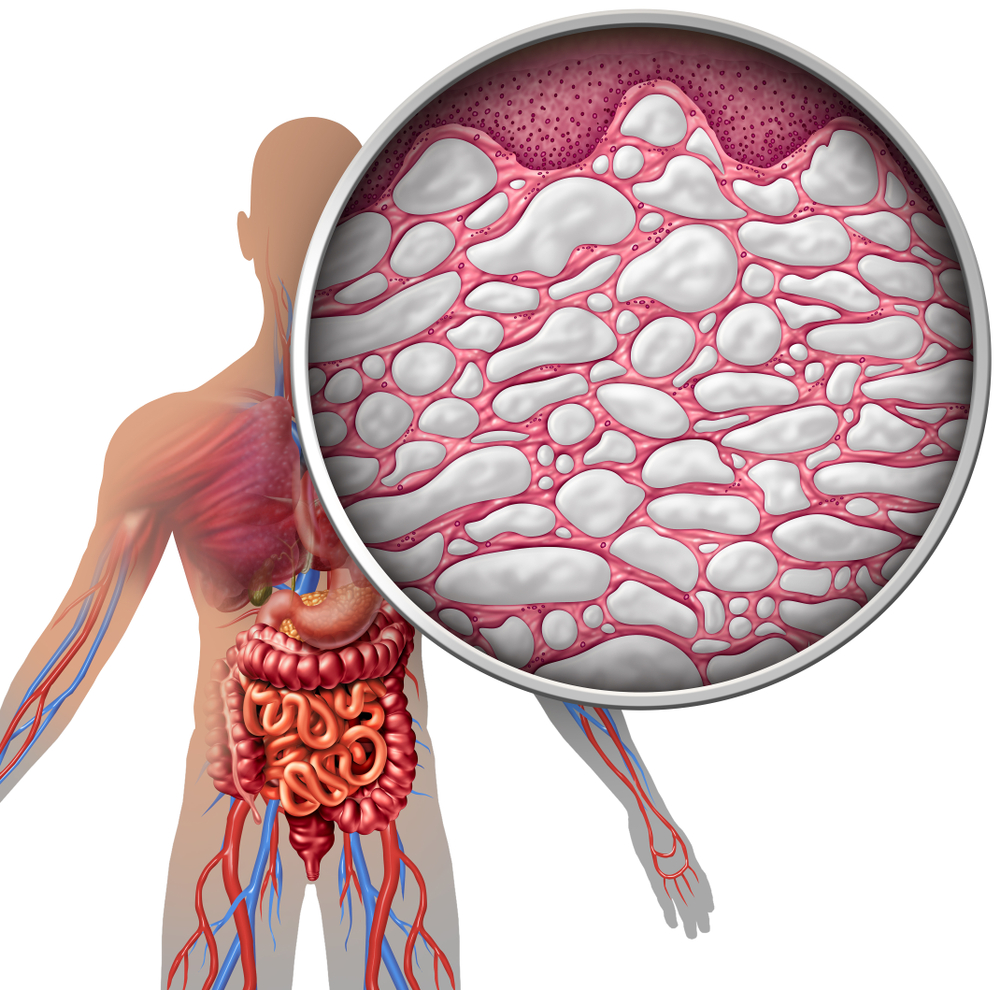
So what is fascia then?
Fascia is comprised of several types of collagen, elastin, Extra-Cellular-Matrix, and interstitial fluid. Kumka describes and defines 4 main categories of fascia in the above article: linking fascia, fascicular fascia, compression fascia, and separating fascia. The new discovery called the interstitium focuses on “holes in the fascia” that contain interstitial fluid and is linked to the lymphatic system. Dense bands of collagen hold the interstitial fluid in place via surface tension and capillary action; kind-of like the inside of a sponge. The interstitium runs in and around many different structures all throughout the body including the lungs, lining the digestive tract and even surrounding muscles. All of the components of fascia and the interstitium fall into the category of connective tissue.
Why do people want to classify the interstitium as an organ?
Mainly? It’s just much more alive than previously understood. It comes down to the fact that we have new ways of looking at this tissue under a microscope. The “discovery” of a “new organ” called the interstitium is really due to a histologist discovering a new way to view fascia under a microscope without needing to smash it and distort it. It does not change or modify our current understanding of the role of the fascia. Sue Hitzaman, the creator of the MELT method had this to say about the interstitium “I like this word interstitium. But let me assure you, there’s not much new about it.” Probe-based confocal laser endomicroscopy is the new technology that allowed researchers to see the interstitium. I find these new kinds of technology very exciting!
We have known about fascia for a long time now. And fascia is almost everywhere in the human body. Fascia is the stuff that holds us together, literally; and it has a multitude of functions. Fascia is essentially a web of bands or sheets of connective tissue. It covers and wraps the internal structures of the human body. Dr. Kumka says “Fascia is virtually inseparable from all structures in the human body and acts to create continuity amongst tissues to enhance function and support.” Fascia and the muscles it surrounds are what make our kinetic-chains. Fascia is what links our muscles together so that they can work as a functional unit.
So fascia isn’t just connective tissue then?
Not at all. Many of us have already put two-and-two together before this big news. We worked with the understanding that fascia, extra-cellular-matrix (ECM) and the associated interstitial fluid all work together and play an important role in nutrient delivery and lymphatic drainage in addition to the obvious structural support. We also already understood that this space played an important role in nerve conduction and somatosensory signaling such as proprioception. But for many, the discovery of the interstitium and its function may be a profound new concept that broadens their understanding of fascia in general and how vital it is for our total health and performance. Regardless, it is great to see fascia getting so much attention.

What kind of fascia-related disorders do you see and treat?
A big problem that I treat is fascial adhesions. An adhesion is when fascia gets stuck to other structures around it. When you stretch and feel those tight areas that pinch and pull, that’s often the “stuck” fascia. So when you wake up every morning and stretch, that feeling is the undoing of all the small adhesions that formed in your fascia while you were sleeping.
Does stretching break up adhesions?
Yes, to a certain degree. But you know what I’m about to say to this – we talk about it all the time. Stretching can break up small adhesions. But much of the effect from static stretching comes from a resetting of the pain threshold within the muscle-tendon units. To break up adhesions fully requires deep myofascial release techniques like IASTM. As I’m fond of saying, you can’t undo a knot by pulling on it. Sometimes you’ve got to push it to loosen it. The same applies to muscles and adhesions!
What problems do adhesions cause?
One of the main problems that fascia adhesions cause is pain. When you’ve been sitting or immobile for a long time, you begin forming adhesions. Then when you try to move and be active, you feel these adhesions as stiffness and pain. I find that providing fascial treatment and encouraging mobilization in my clients can work wonders when it comes to chronic pain and stiffness. But adhesions dramatically affect athletic performance in many ways. The two most concerning and impactful would have to be the way adhesions affect our biomechanics and the way they affect force production, a.k.a. strength!
Think of biomechanics simply as the path your joints take through a particular movement. What path does your shoulder take as you lift your arm over your head? Where did you feel tight? Did you feel a pinch? If you change the path, are you less tight or does the pinch go away? What if you can’t get the pinch to go away no matter how you change the path your arm takes?
Well, you might have a torn rotator cuff, hahaha! Or you might have adhesions throughout your shoulder girdle preventing it from tracking correctly. And maybe this is causing impingement of your rotator cuff. When you have adhesions in the muscles and fascia around a joint, joint motion will be affected. If you have adhesions in your upper traps your shoulder health can become seriously compromised.
That’s a great point. We are going to publish an article about shoulder impingement in the near future. So people who want to learn more about shoulder impingement can add their email to our mailing list and get this and other articles sent directly to them.
Tell me how adhesions decrease strength.
The other major way adhesions affect athletic performance is by decreasing the amount of force a muscle or set of muscles can generate. Yes, adhesions can make you weaker! Every muscle is comprised of a hierarchy of structures that form the muscle. We can put an illustration here in the article to show you all the anatomy that we are talking about.
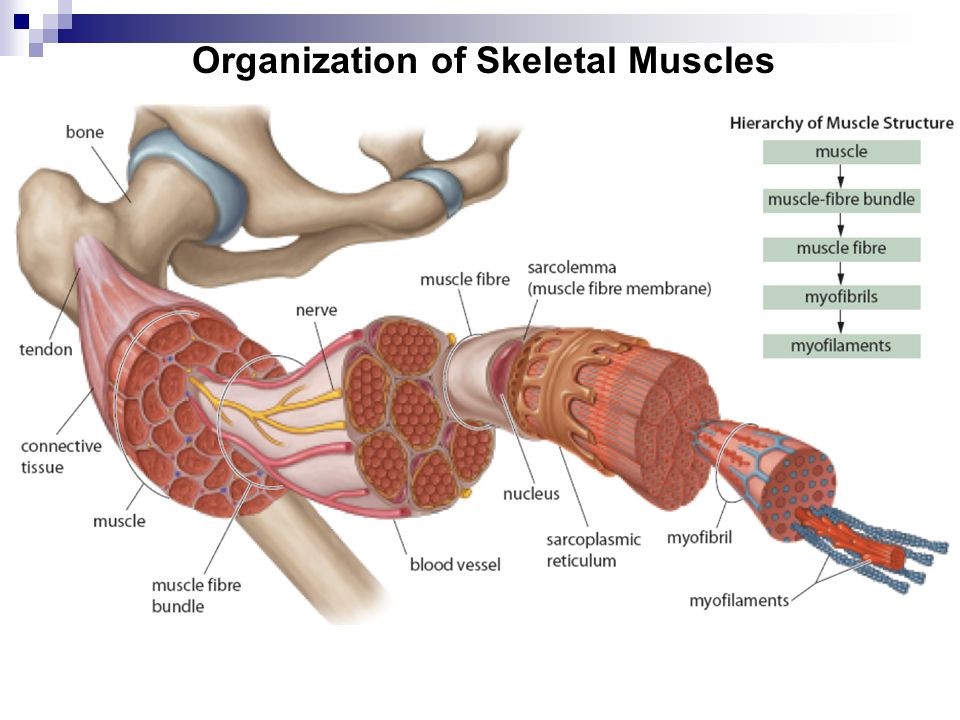
So as you can see in the illustration, there are A LOT of fibers, filaments, and myofilaments that make up our muscles. And each of these structures is wrapped in fascia that can become stuck to structures around it. Huge sections of muscles become adherent to itself if these intramuscular adhesions are left untreated. Then those fibers can’t fire independently. And that greatly limits how well your muscles can do their job. Think of it like this: if 30% of your muscle is full of adhesions, then only 70% of your muscle is contracting optimally.
True! All the fibers in a muscle don’t contract all at once. So If you glue them together they won’t be able to work the right way. (If you’d like to learn more about the way your muscles actually fire, check out this prior post.)
As an athlete, can I prevent adhesions?
Yes and no. Adhesions forming between our fascia and muscles is a natural part of the human condition. Think about how stiff you get during a 3-hour car ride or the stiffness you feel in the morning when you wake up and start moving. There is an innate expansion and tightening within our fascia and interstitium, and it can’t be avoided. Dr. Gil Headly does a fantastic job explaining this in his famous speech “The Fuzz.”
The best practice is to keep this natural process of tightening and loosening as minimal as possible. Because once the adhesions become too thick, they will need to be treated in other ways. We can prevent major adhesions and scar tissue from forming by being active and mobile. But the smaller adhesions that occur while we sleep or sit in the same position for hours is simply part of this experience. Staying hydrated plays an important role in the prevention of adhesions too.
That’s a great video by the way. It’s something I work with every time I’m in surgery. One of the ways in which I see this concept most demonstrably is with Trochanteric Bursitis. When it’s severe, I may have to do a bursectomy. Now I can’t really remove a bursa, because it is supposed to be an empty space, and a normal bursa has just a little bit of this “fuzz.”
But with bursitis, it becomes incredibly thick and glues the fascia to the bone and muscle. So what I do is remove that thick adhesive tissue and make an empty bursa once again. You can see a video of me performing an arthroscopic trochanteric bursectomy on my YouTube Channel here.
So what are some ways we can treat fascial adhesions then?
We treat fascial problems in a multitude of ways. Foam rollers and mobility balls really help to get that stuck fascia unstuck. (For more information on these methods of self-myofascial release, check out this article on How Foam Rolling Works as well as our article on 8 simple Foam Roller Exercises.) And a massage can treat fascial problems too. So can other manual therapy techniques. Using devices such as the Myobuddy Pro (readers can use the code EPIC100 at checkout for $100 off) or the Theragun are effective in the treatment of adhesions and scar tissue also. Dry Needling and Cupping are two other modalities that therapist use in the treatment of fascial problems.
Now one of the most successful and effective methods of treating fascial problems is Instrument Assisted Soft Tissue Mobilization (I.A.S.T.M). IASTM utilizes tools manufactured from stainless steel shaped to the body’s contours to break up adhesions. These tools allow me to work on all the various curves and ridges of the body. I work the tissue to shape and align fascia while breaking apart adhesions allowing optimal blood flow and hydration to return to the area.
Of course, it is vitally important that treatment of fascial restrictions be followed with optimal and effective movement patterns during daily activities and exercise. Once you have reduced the adhesions with one of the treatments described above healthy functional movement is key in preventing them from coming back.
Yes! You don’t want to be one of these people that goes to the gym in the morning and then sits at a desk for 8 straight hours. Then they wonder why they get so stiff and sore! I like to call that the “Anti-Mobility WOD.”
So is there anything else we should know about fascia and interstitium?
It’s really important to know and understand that your fascia and interstitium are just as important to train and maintain as any other major component of the human body. They may even be one of the most important aspects of health, vitality, and performance. So, let me ask you… How do you train your fascia? And how healthy is your interstitium?
Personally, all of these techniques have become a vital part of my recovery and maintenance. The awkward positions that I have to work in while operating really create some abnormal movement patterns. And lifting with those abnormal patterns led to some significant pain and injuries. Plus being 6’8″ tall means that the ergonomics of this world aren’t designed around me. My wife thinks I should be classified as “megafauna!” Hahaha!
But since I’ve been working on stretching, mobility, and fascial work I find that move and feel much better than I ever did before. While I may not have perfect movement patterns or be the most flexible person in the world, I’m continuing to work on it. I use a foam roller every time I’m in the gym. I often use a foam roller or mobility ball after work to help stretch out. And I try to get all the way down in a deep squat when I can, just to keep the lower body as flexible as possible!
Anyway, Scott, it’s been great talking with you. And thanks for providing our readers with some great insights into a part of their body they probably pay too little attention to!
Any time man! Thanks for talking with me!
Scott Dolly can be found at his home website http://www.evolutionhpr.com/
You can also catch him geeking out over fascia and fitness on these awesome podcasts:

