What is trochanteric bursitis?
Trochanteric bursitis is a common cause of hip pain. Trochanteric bursitis is traditionally described as an inflammation of the bursa at the lateral side of the hip. Pain is usually over the bony point of the hip known as the greater trochanter. Most physicians will tell you that simply relieving the bursitis is all that’s required to stop the pain of trochanteric bursitis.
But after years of taking care of hip pain and operating on trochanteric bursitis, I no longer think that inflammation is the major cause of long term problems with trochanteric bursitis. Inflammation plays a role at first, but it merely sets the stage for the real cause of chronic trochanteric bursitis.
So what’s the REAL cause of trochanteric bursitis? And what can you do about it? Well, that’s what this entire article is about, my friend!
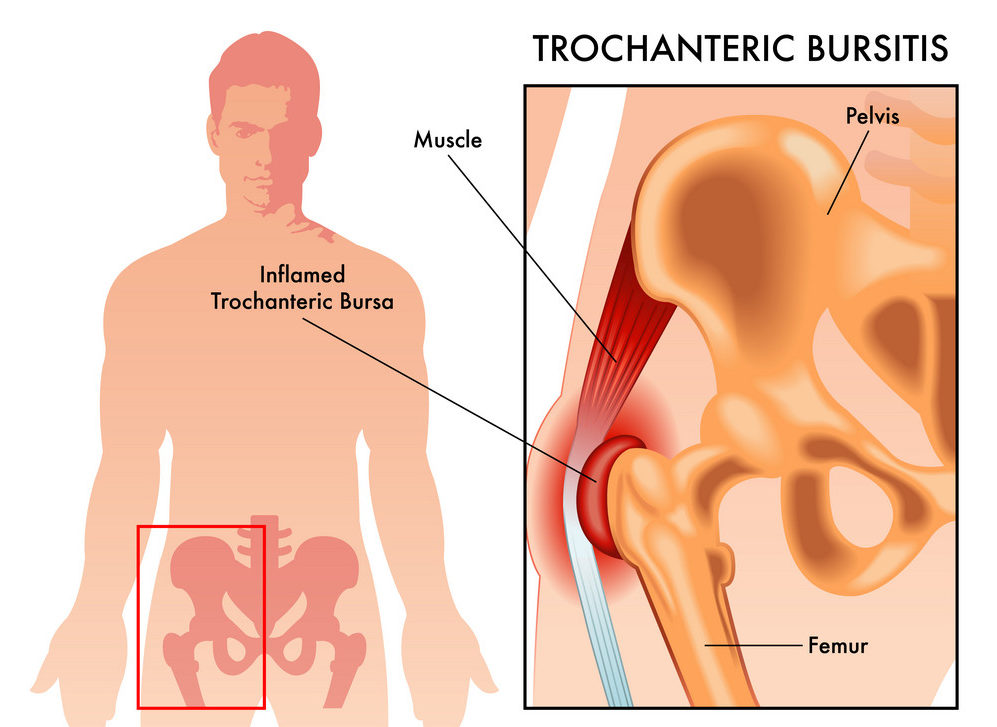
How does trochanteric bursitis start?
All trochanteric bursitis starts with some kind of injury, either acute or chronic. As a surgeon specializing in sports medicine, I see a few cases of bursitis in some active adults between thirty and fifty years of age. But that’s not common. Most of the time, hip bursitis is a problem that we see in adults 60 and over. And while all cases of trochanteric bursitis may wind up similar, the starting causes can vary quite a bit:
Direct Injury
This can include falling onto the hip, bumping the hip into an object, or lying on one side of the body for an extended period. A car accident or major fall can be the cause in younger people.
Chronic Injury
Repetitive activities might include running, climbing, or standing for long periods of time. I see a few functional fitness athletes with this problem, but it’s rare. But in that age group, it’s most common in long-distance runners.
Spinal Disease
This is a very common problem in our older patients. Arthritis of the lumbar spine and scoliosis are quite common in patients with trochanteric bursitis. But we’ve never been sure which is the chicken and which is the egg: does spine disease cause trochanteric bursitis? Or do they both come from an unidentifiable common cause? Or does the lack of mobility from spinal disease lead to progressive bursal adhesions? My bet is on the latter. Read further to find out why I think this.
Inflammatory Diseases
Rheumatoid arthritis, gout, or psoriasis can cause hip bursitis too. Calcific bursitis would fall into this category as well. We don’t know why some people get calcific bursitis or tendinitis, but there does seem to be a genetic predisposition. These diseases aren’t injuries though, but rather situations where your body’s immune system attacks the tissue around the joints and muscles, leading to inflammation.
But most of the time, we don’t even know how a patient’s bursitis began. And as you can see, many of the known causes deal with inflammation. But if inflammation was the only problem, we could relive bursitis with oral anti-inflammatories or injections. So why don’t they always work?
The REAL cause of trochanteric bursitis
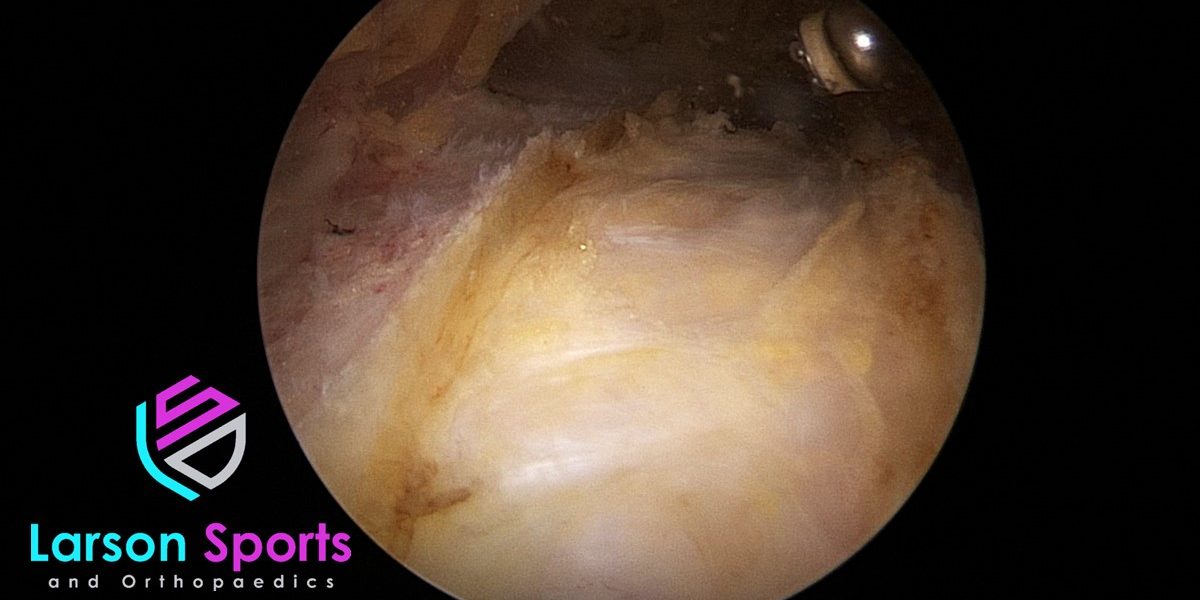
I believe the reason that anti-inflammatory medications don’t always resolve this problem because the process has entered the second phase. That’s what I think of as chronic trochanteric bursitis. This chronic phase is characterized by the production of thick adherent connective tissue filling the bursa. These adhesions grow between the different structures around the bursa and glue everything together. And that’s where the real problem lies. You can check it out in this video. WARNING: this is an actual video of an arthroscopic surgery that I’ve narrated for you all, to show you some of the adhesions that I’m talking about, as well as the bursa and what it looks like.
What is a bursa?
To understand why the scarring of the bursa could cause problems, you have to understand what a bursa is. Look at any anatomy book and you will see the bursa drawn as little blue bubbles. We describe them as fluid-filled spaces that allow tissue to slide over each other. But that is just plain wrong.
A bursa is simply an area between to planes of tissue that has few if any fascia connection. Between each muscle, bone, tendon, organ, and ligament in your body, there are small fibers of collagen, connecting your entire body in a web of tissue that some now consider to be an organ in it’s own right.
In some areas, these connections need to be firm and solid to keep organs, muscles, and other tissues in a certain location.
But in other areas, the tissues need to move freely from one another. So in those areas the connective fascia is sparse and thin, almost like spiderwebs. And that’s what a bursa REALLY is: just a loose plane between two body structures with few fascial connections. That’s because they have different jobs and need to move in different ways.
Why Do We Have Bursa?
The trochanteric bursa is a great example of why we need bursa. The IT band is a support structure, used to balance the side of your leg and pelvis like the cables on a suspension bridge. It needs to stay stable. But the trochanter and all the muscles attached to it need to move in many directions to allow for a full range of motion at your hip. Those muscles have places to go and things to do. Think of them like the cars on the same suspension bridge.
If the cars get stuck to the bridge, they can’t do their job. And that’s why the adhesions of late-stage bursitis cause problems: Two tissues that have different jobs and need to move in different ways are now tethered together and pain is the end result.
What are the symptoms of trochanteric bursitis?
Trochanteric bursitis symptoms are usually pretty classic. Symptoms typically include the following:
- Pain on the outside of the hip, sometimes radiating into the thigh or buttock.
- Soreness lying on the affected side, especially problematic at night.
- Pain when you push on the outside of the hip.
- Sitting for long periods can cause pain, especially if the seat is firm.
- Pain on the side of the hip when walking, especially long distances or going up stairs.
If your symptoms don’t match these ones, check out my other article: Hip Pain While Squatting. You can find my entire list of common problems of hip pain to see if they match your symptoms better.
How do you prevent trochanteric bursitis?
Because most cases of bursitis are caused by overuse, the best treatment is prevention. It is important to avoid or modify the activities that cause the problem. Stay mobile and flexible, but don’t overdo things. When you notice that your workout is causing hip pain, take a break and stop doing the exercises that cause pain.
You should also correct the underlying problems like leg length differences, spine disease, poor posture, or poor form when working out. And be sure to stretch and mobilize regularly. Using a foam roller and working on hip stretching before and after workouts.

How is trochanteric bursitis treated?
Usually conservative treatment of trochanteric bursitis is pretty effective. This is especially true when you seek treatment EARLY. Injections, pain relief, and physical therapy are the mainstays of treatment. But if the adhesions are too thick, we sometimes need to release them with surgery.
Injections
When in the early inflammatory phase, injections can be very effective. I often use Toradol when I inject a painful bursa, instead of steroids. Toradol is a non-steroidal anti-inflammatory medication. I like it better than steroids because repeated steroid injections have been known to lead to tendon tears. You don’t need gluteus medius tears in addition to the bursitis.
Physical therapy
This is also very effective early on. The goals of therapy are to strengthen the hip muscles, mobilize the soft tissues, and correct any underlying problems. Predisposing problems can include pelvic tilt, poor posture, leg length differences, and gait disturbance. Foam rolling, IASTM, and manual treatment modalities can also help keep the tissues free of each other.
Pain Relievers
These are also important since trochanteric bursitis can make it difficult to get any quality sleep. Some of the best ways to relieve the pain of trochanteric bursitis include:
- Anti-Inflammatories (ibuprofen, motrin, tylenol) if you can take them.
- Try anti-inflammatory supplements if you can’t take the medications above. One of the best options is Turmeric (make sure you get it in either liposomal form or with Bioperine in order to aid absorption.)
- Lidocaine patches: These can really help decrease pain just below the skin. They work pretty well on shoulders, trochanteric bursitis, and back pain.
Surgery
Surgery is a last resort. But it can be very effective at relieving pain from trochanteric bursitis. As you can see from the video above, surgery is usually done through a couple of small incisions, arthroscopically. Doing these arthroscopic trochanteric bursectomies is what made me realize the error of our theories about the disease. This surgery doesn’t remove inflammation. I simply free up the two layers and remove the garbage that has grown between them.
And that led me to think about the REAL reason behind trochanteric bursitis. It’s not inflammation. At least not in the long term. The long term problem is those adhesions that grow between the IT band and everything below. Early on, you need to get rid of the inflammation and keep the adhesions from forming. But once the adhesions are there, you need to break them up to have any hope of relief. Whether you break the adhesions through surgery or other means, it’s the best way to address chronic trochanteric bursitis.
If you live in Virginia, Maryland, or West Virginia and think you may need surgery for trochanteric bursitis please call my office for an evaluation.
References:
Conservative treatments for greater trochanteric pain syndrome: a systematic review
Efficacy of treatment of trochanteric bursitis: a systematic review
Disclaimer, there are some affiliate links on this page. These return a small percentage of your purchase to help keep this website running, but it does not increase your costs at all.