Piriformis syndrome is a rare problem that I have actually ended up seeing fairly regularly. That’s because I’m a surgeon specializing in sports medicine and hip disorders. So I see a lot of people diagnosed with labrum tears of the hip, and a certain percent of them are actually piriformis syndrome that was misdiagnosed as a labrum issue. Plus, piriformis syndrome is more common in runners, weight lifters, and cross-fitness training. So I’ve learned quite a bit about diagnosing and treating this common disorder.
It is important to note that piriformis syndrome is a rare issue. If you have the kinds of symptoms we describe in this article, it’s much more likely that you have a problem in the spine itself. Disc herniations, sacroiliitis, spine arthritis or other disorders are far, far more likely to be the source of these symptoms. Check out my other article about the different sources of hip pain ( Hip Pain When Squatting ) to see if any of them match your symptoms more closely.
One of the more common problems I’m asked about is hip pain people feel when squatting. So I’ve written this entire article talking about the most common causes of hip pain when working out. Check here for other causes besides piriformis syndrome.
Cause of Piriformis Syndrome
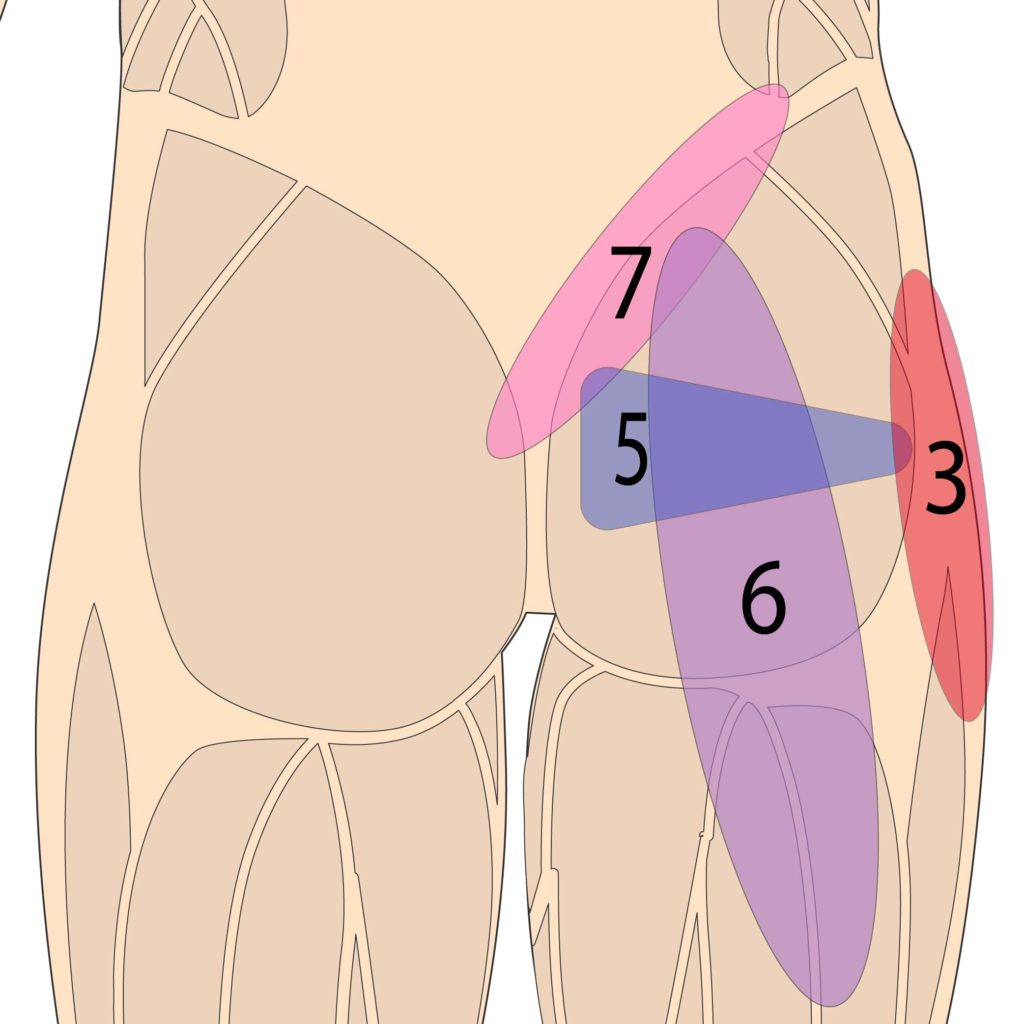
The piriformis is a muscle deep in the back of the hip. It helps with the fine control and external rotation of the hip. And it lies directly over the sciatic nerve. Piriformis syndrome occurs when the sciatic nerve gets squashed under the piriformis when the muscle gets tight or spastic. This is usually due to chronic overuse. But people with piriformis syndrome also have a high likelihood of abnormal sciatic nerve anatomy.
The sciatic nerve is a thick and long nerve in the body. Normally it passes under the piriformis muscle in the buttock, goes down the back of the leg, and eventually branches off into smaller nerves that end in the feet. The most common cause of sciatica or sciatic nerve entrapment is a herniated disc in your lumbar back. But arthritis in the spine or bulging discs can cause these problems as well.
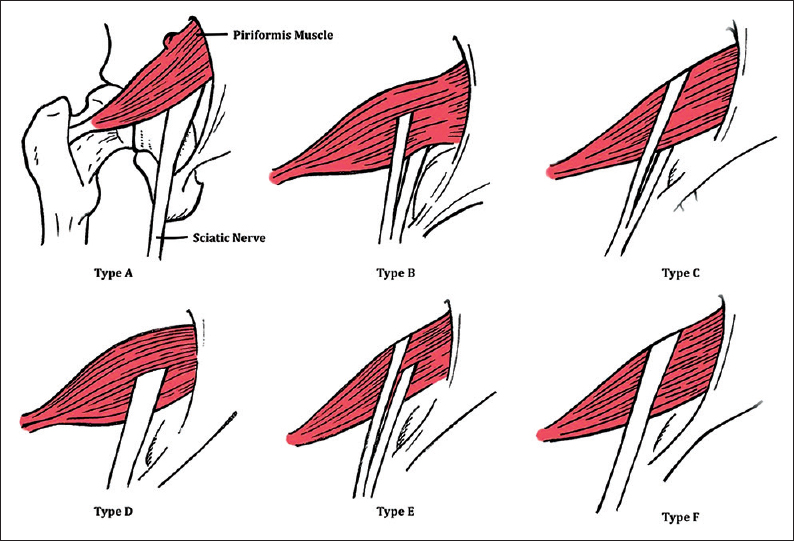
The images below show the most common variation in the anatomy of the sciatic nerve and piriformis muscle. Of course, this comes from studies in people who’ve had surgery for piriformis syndrome. As you can see, the nerve can pierce the muscle, come out over top instead of under it, or split into halves and encircle the piriformis. When I operate on patients with piriformis syndrome, I’ve most commonly seen nerves that split into two halves or ones that pierce the muscle itself.
Piriformis Syndrome Signs and Symptoms
- Pain and spasms in the buttock
- Numbness in the buttock, leg, or foot
- Tingling feeling (pins and needles) in the leg
- Cramping in the buttocks
- Difficulty sitting on the affected side
- Pain is worse after running or squats
Piriformis syndrome usually starts with pain deep in the buttock. Later signs of piriformis syndrome may include pain down the length of the sciatic nerve, as far as the foot. People experience severe buttock pain and/or leg pain. And you can also get muscle spasms, cramps, charlie horses, or muscle quivers.
The pain is due to the piriformis muscle compressing the sciatic nerve. It is often worse when sitting, especially if you keep a wallet in the same pocket. Pain may be triggered when running, while climbing stairs, stretching the piriformis, exercising, or sitting for long periods of time. The symptoms often fluctuate in severity, depending on how you sit or stand and what activities you’ve been doing. Long car rides can be a real killer!
Piriformis Syndrome Diagnosis
Unfortunately, there is no definitive test for piriformis syndrome. X-ray, MRI, and nerve conduction studies can all be negative with piriformis syndrome. I usually have to make this diagnosis based on the combination of symptoms, the kinds of activity you do, and the physical exam. When I do tests like an MRI, it’s mainly to rule out other more common problems that could cause these symptoms. You can’t see the sciatic very well on a hip MRI, so it’s not a reliable way to diagnose this problem.
Piriformis Syndrome Treatment
Prevention
I see a lot of people with very tight piriformis muscles at the gym. Working out a muscle regularly can lead it to become fairly tight and lose flexibility. And since “every day is leg day” your hips can get very stiff if you don’t incorporate stretching into your daily routine. The best way to target this muscle is with the Piriformis Stretch. Make sure to do this a couple of times each week to help prevent piriformis syndrome from developing. Deep tissue massage, heat, trigger point balls, and other similar mobility aids can help a lot too.

Treatment of Early Piriformis Syndrome
When you start developing the symptoms of piriformis syndrome, you want to start treatment quickly. See your doctor and look into their treatment options. Primary treatment consists of resting the muscle (stop the running, biking, burpees, squats, and deadlifts) and getting into physical therapy. A physical therapist can do soft-tissue massage to the gluteal and lumbosacral areas. They can assess muscle imbalances and exercise form. They can also administer heating packs, manual manipulation, passive stretching, dry needling, electrical stimulation, and other treatment options.
A doctor can also order injections of the piriformis muscle, which are usually done by an interventional radiologist. Muscle relaxers and steroids can also be pretty effective. Your doctor can investigate all the other potential sources of pain. And they can get you to surgery if needed.
Recovery Phase
If the therapy is successful, or if you’ve ended up with surgery, the next phase is recovery. Pressure on a nerve causes damage that isn’t immediately fixed by surgery. Taking the pressure off the nerve simply prevents further damage from occurring and allows the nerve to begin healing on its own. It’s normal for numbness and tingling to persist for weeks or months after the pressure is gone. Physical therapy is enhanced during the recovery phase; the goal is to strengthen the hip muscles and to optimize pelvic alignment and tilt.
Maintenance Phase
Because many people who develop piriformis syndrome are athletes, they should slowly resume training over a period of several months. If not, it could come back quickly. Go easy on the distance; you don’t want to start training for marathons as soon as you are done with therapy. You should also get back into glute strength training slowly. That includes exercises like squats, kettlebell swings, sled push, deadlift, and GHDs. You can start doing these again but take it easy. Otherwise, you’ll end up pushing yourself back into full-blown piriformis syndrome.

massage ball set 
lacrosse balls 
textured massage balls 
spiked massage ball 
trigger point set
Surgery For Piriformis Syndrome
Surgery is a last resort, as usual. Technically, it is a relatively simple surgery, because it’s similar to how we start hip replacements. Except we don’t usually mess with the nerve during a hip replacement. We leave it safely beneath the other muscles.
The tricky part with piriformis release surgery is that we have to actually operate around the sciatic nerve and release the tissue around it. And nerves don’t like to be operated on… or touched… or looked at. So not many orthopedic surgeons are willing to risk working in this area. So a lot of other surgeons refer these patients to me for piriformis release.
Conclusion
Piriformis syndrome may be an uncommon cause of butt and leg pain. But it can be very problematic and debilitating. Fortunately, it usually responds well to stretching and physical therapy. But if you need further treatment, call an orthopedic surgeon. And if you live in Maryland, Virginia, or West Virginia I’m not that far away. You can contact my office on our website: Bone and Joint Specialists of Winchester.
References
- Piriformis Syndrome: A Narrative Review of the Anatomy, Diagnosis, and Treatment.
Anatomical variation in bifurcation and trifurcations of sciatic nerve and its clinical implications. - Diagnosis and Management of Piriformis Syndrome: A Rare Anatomic Variant Analyzed by Magnetic Resonance Imaging.
- Piriformis syndrome: a cause of nondiscogenic sciatica
- Four symptoms define the piriformis syndrome: an updated systematic review of its clinical features.

Dr. James Larson is an orthopedic surgeon specializing in sports medicine and arthroscopic surgery. He also holds a CF-L1 certificate and is a Certified BFR Specialist. He supports weight training and high-intensity exercise throughout the lifespan. He started LSO to keep more people moving better, longer.

